
What’s wrong with your skin? Are those bug bites? Do you have burns? Is that contagious? Does it hurt? If you have psoriasis, you have probably fielded those painful questions and more. While most people do not mean any harm, they are alarmed by the sight of your reddened skin and scaly silver plaques. Effective treatment at Associates in Dermatology in Westlake, OH helps you find relief and enjoy other topics of conversation other than your skin condition.
What is psoriasis?
While psoriasis symptoms present on the skin, the disease is a chronic autoimmune disorder. It occurs when the immune system erroneously speeds up the turnover of skin cells. Excess cells quickly accumulate in patches called plaques, characterized by inflammation and excessive shedding.
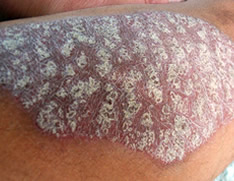
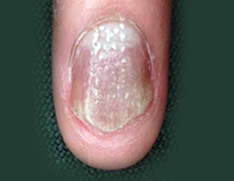
Plaques often develop at the elbows and knees but may occur anywhere, including feet, palms of hands, scalp, and genitals. Fingernails and toenails may also be affected.
What causes psoriasis of the skin? There appears to be a genetic component, with outbreaks triggered or aggravated by:
- Certain medications
- Excessive consumption of alcohol
- Infection
- Injury
- Smoking
- Stopping corticosteroid treatment
- Stress

Psoriasis types include plaque; guttate causing a multitude of small red spots; and a severe form called pustular with white bumps surrounded by red skin. Up to 30 percent of individuals with psoriasis also have a related form of arthritis, in which the immune disease attacks joint tissues as well as skin.
Seeking treatment for psoriasis in Westlake, OH
If you have struggled with the condition, you probably wonder how to get rid of psoriasis once and for all. Since psoriasis is chronic, there
Clearing skin on the scalp may be as simple as using a special psoriasis shampoo, with moisturizers and ointments to soothe skin. Mild cases may be managed with topical corticosteroids or by taking a vitamin D3 supplement. Drugs may be used to moderate the immune system, and many new injected biologic treatments are available to treat severe psoriasis and psoriatic arthritis.
Many patients prefer phototherapy – medically supervised application of ultraviolet light to clear plaques. This technique avoids the risk of systemic side effects possible with medications.
Call Associates in Dermatology at (440) 482-8323 for a one-on-one psoriasis management plan. Remember, we have offices in Lorain and Middleburg Heights, too.













